These are some of the conditions that our professional allergists treat.
Allergic Rhinitis
This is common known as hay fever and affects more than 20% of United States citizens. Allergic rhinitis is caused by exposure to airborne allergens such as pollen, dust mites, pet dander, or mold. These allergens are ignored by the immune system and people with allergic rhinitis have reactions because their immune system mistakenly identifies these allergens as intruders.

Animal Allergy
Allergic reactions to animals can be a significant cause of severe allergic symptoms. The protein allergens (allergy causing substances) from animals are contained in the sebaceous glands of the cat’s skin or in the dander (the surface layer of skin cells), saliva or urine of dogs and rodents. The allergen particles are so small they cannot be seen in the household environment, but eventually they penetrate the rugs and bedding. Animal fur itself is not considered to be a major cause of allergy.

Dust Allergy
Although there are many components in house dust to which people may become allergic, the most important is the dust mite. This is a microscopic mite which is found in homes. Dust mites live primarily in carpets, mattresses, pillows, box springs and upholstered furniture. They thrive in humid and warm conditions and feed on shedded human skin! The waste products produced by dust mites are highly allergenic. Each dust mite produces about 20 waste particles each day. These particles continue to cause allergic symptoms even after the mite which has produced them has died. In addition, house dust contains molds, pet and human dander and cockroach waste which may be allergenic.

Mold/Fungus Allergy
Molds (fungi) are a lower form of plant life which cannot make their own food and therefore must feed on living or dead organic matter. Molds can grow on anything and require no sunlight for growth. They thrive in total darkness in the ground, caves, or tree trunks. Mold spores are spread by the wind, insects and man. These sports are difficult to totally escape but excessive exposure can be avoided.

Asthma
For those living in Cincinnati, Asthma treatment is available through the dedicated physicians at Bernstein Allergy Group, Inc. Millions of Americans are afflicted with this condition, but many do not know what triggers it. Many, in fact, do not even know what happens to their own bodies when they have an attack. We make it our job to inform every patient who walks in our door about what it truly mean.

Occupational Allergies
Occupational allergies refer to nasal, lung or skin reactions that occur as the result of exposure to one or more agents in the workplace. These reactions may be the result of developing sensitizing IgE antibodies to a specific agent or may occur through other non-IgE mediated mechanisms of action. Sometimes a specific causative agent is not obvious or readily identifiable. If you suspect you are developing symptoms in the workplace, the Bernstein Allergy Group doctors have extensive expertise in evaluation, diagnosis, treatment and management of occupational respiratory and skin diseases.

Chronic Hives (Urticaria)
Hives or urticaria can be defined as a red rash with itching, swelling and elevation of the skin. Hives can be accompanied by more severe swelling which can occur underneath the skin, especially in the soft tissues around the eyes, lips, hands and feet. This form of swelling is referred to as angioedema. Hives and angioedema may occur alone or together. Both may occur suddenly in the form of a reaction to a drug such as penicillin, an infection such as hepatitis, or after a sting by an insect. Certain foods such as eggs, peanuts, tomatoes, walnuts and fish can cause allergic reactions which can be manifested by the appearance of hives and angioedema.
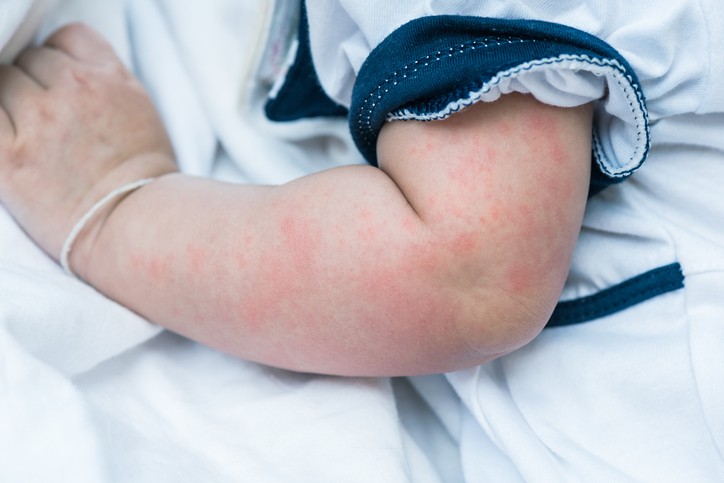
Drug Allergy
Just about any drug can cause an allergic reaction. Penicillin antibiotics and penicillin like drugs represent the most common causes of drug allergies. Allergic Drug Reactions to penicillin can range from mild rashes or hives to life threatening allergic reactions, otherwise referred to as anaphylaxis. Some of the other drugs which commonly cause allergy are sulfa antibiotic drugs (Bactrim, for example), the seizure drugs (dilantin, for example), as well as anticancer treatments. Unlike penicillin, there are no specific tests for most of these drugs. In general, doctors will advise patients to avoid a drug to which they have experienced an allergic reaction. This is very good advice for most drugs that have caused serious reactions in the past.

Food Allergy
Food allergies are occur because of an immune system reaction to certain foods. 1 in 20 Americans are affected by food allergies and can occur at any age, but most commonly in babies and young children. 90% of food allergies are related to milk, egg, soy, wheat, tree nuts, peanuts, shellfish and fish.

Environmental Allergy
Our environment, whether it is our homes, schools, or workplaces, they all contain potential causes of environmental allergies. The best thing you can do is avoid these allergens, however it is easier said than done. Many allergens are airborne such as plant pollen, mold, or other substances. Our allergists can provided information that can help you decrease your exposure to these allergens. There are also treatment options we can provided that will help reduce your sensitivity to those allergens that affect you.

Anaphylaxis
Anaphylaxis is a life threatening reaction where multiple organ systems are involved leading to symptoms of hives, angioedema, wheezing, shortness of breath, chest tightness, cough, nausea, vomiting, diarrhea, dizziness and in extreme cases loss of consciousness and death. Anaphylaxis can occur after exposure to a food, stinging insects, drugs and a host of other agents that you may or may not know you are sensitized to. Sometimes anaphylaxis can occur spontaneously without any known cause. If you have had an anaphylactic reaction or are at risk for one, it is important that you be evaluated and managed properly to avoid unnecessary adverse outcomes. The Bernstein Allergy Group, Inc. physicians have extensive experience in the evaluation, diagnosis, treatment and management of anaphylaxis.

Angioedema
Angioedema or “soft tissue swelling” occurs as the result of fluid accumulation in the deeper dermis. Angioedema occurs by itself in 20% of cases and in conjunction with hives in 40% of cases. Isolated angioedema can often be seen as a result of certain medication reactions such as ACE inhibitor blood pressure medications or aspirin and/or non-steroidal anti-inflammatory medications (Advil or Aleve). Isolated angioedema is also seen in patients who have rarer conditions called hereditary and acquired angioedema. Patient with hereditary angioedema have either a decreased amount of C1 Esterase inhibitor or functionally abnormal levels. This enzyme is important for regulating the production of a mediator called bradykinin that can cause swelling if there is too much in the body.

Chronic Obstructive Pulmonary Disease (COPD)
Chronic obstructive pulmonary disease (COPD) refers to a group of lung diseases that block airflow due to lung damage and make it increasingly difficult to breathe. Unlike asthma, obstruction of the lungs that develops in COPD patients does not improve and is not fully reversible. Emphysema and chronic bronchitis are the common conditions that make up COPD where the normal exchange of oxygen and carbon dioxide are impaired.

Occupational Disorders
– Occupational Lung Diseases (occupational asthma)
 Allergic respiratory diseases in the workplace, like occupational asthma (OA), represent a significant public health concern leading to long-term health consequences and socioeconomic costs for the affected worker, employer, and society as a whole. The lungs are particularly vulnerable to contact with these types of exposures due to their extensive surface area, high blood flow, and thin alveolar epithelium. Occupational asthma is the most prevalent occupational lung disease in industrialized countries and since undiagnosed OA can cause considerable medical and economic consequences, aggressive prevention strategies are essential. Despite an increase knowledge of sensitizing agents in the workplace as well as improvements in workplace safety and reporting, OA continues to afflict workers worldwide.
Allergic respiratory diseases in the workplace, like occupational asthma (OA), represent a significant public health concern leading to long-term health consequences and socioeconomic costs for the affected worker, employer, and society as a whole. The lungs are particularly vulnerable to contact with these types of exposures due to their extensive surface area, high blood flow, and thin alveolar epithelium. Occupational asthma is the most prevalent occupational lung disease in industrialized countries and since undiagnosed OA can cause considerable medical and economic consequences, aggressive prevention strategies are essential. Despite an increase knowledge of sensitizing agents in the workplace as well as improvements in workplace safety and reporting, OA continues to afflict workers worldwide.
Occupational asthma is caused by inhaling fumes, gases, dust or other potentially harmful substances while “on the job.” Often, your symptoms are worse during the days or nights you work, improve when you have time off and start again when you go back to work. You may have been healthy and this is the first time you’ve had asthma symptoms, or you may have had asthma as a child and it has returned. If you already have asthma, it may be worsened by being exposed to certain substances at work. People with a family history of allergies are more likely to develop occupational asthma, particularly to some substances such as flour, animals and latex. But even if you don’t have a history, you can still develop this disease if you’re exposed to conditions that induce it. Also, if you smoke, you’re at a greater risk for developing asthma.
The allergists at Bernstein Allergy Group can properly diagnose the problem and develop a treatment plan to help you feel better and live better. Once the cause of your symptoms is identified, you and your employer can work together to assure that you avoid exposure to the substance that triggers your asthma symptoms and to high concentrations of irritants.
– Occupational Skin Diseases
Allergic and irritant dermatitis (contact dermatitis): patch testing
Contact dermatitis is the most common occupational skin disease. Work-related skin diseases account for approximately 50% of occupational illnesses and are responsible for an estimated 25% of all lost workdays. These dermatoses are often underreported because their association with the workplace is not recognized. In allergic contact dermatitis, even minute exposures to antigenic substances can lead to a skin rash. Common sensitizing agents include nickel and members of the Rhus genus (e.g., poison ivy, poison oak). Severe skin irritants tend to cause immediate red blisters or burns, whereas weaker irritants produce eczematous skin changes over time. An occupational cause should be suspected when rash occurs in areas that are in contact with oil, grease, or other substances. Direct skin testing (patch or scratch) may help to identify a specific trigger. In workers with occupational skin disease, workplace changes and protective measures are important to prevent future exposure.
Chronic Sinus Disease
– Recurrent sinus infections
– Non-allergic rhinitis (vasomotor rhinitis)
 Non-allergic rhinitis (NAR) is a condition whose mechanism is not as well defined as allergic rhinitis. It is believed to be due to a nerve reflex mechanism which results in changes in the nasal blood flow leading to chronic nasal congestion, post-nasal drainage, runny nose, and sneezing. NAR is triggered by chemical and physical factors such as fumes, tobacco smoke, chemical, and other strong odors, changes in temperature, barometric pressure or changes in body position or eating. Symptoms are usually year round but can improve or worsen depending on an individuals surrounding environment.
Non-allergic rhinitis (NAR) is a condition whose mechanism is not as well defined as allergic rhinitis. It is believed to be due to a nerve reflex mechanism which results in changes in the nasal blood flow leading to chronic nasal congestion, post-nasal drainage, runny nose, and sneezing. NAR is triggered by chemical and physical factors such as fumes, tobacco smoke, chemical, and other strong odors, changes in temperature, barometric pressure or changes in body position or eating. Symptoms are usually year round but can improve or worsen depending on an individuals surrounding environment.
NAR, like allergic rhinitis, can lead to complications such as sinusitis and ear infections. Distinguishing between these nasal disorders is, therefore, very important in order to ensure that correct treatment is recommended. Whereas allergic rhinitis is treated with a combination of avoidance measures, medications, and allergy injections, NAR is primarily treated with medications.
Allergy injections are not indicated for the treatment of NAR. NAR can be severely troublesome for the patient but if treated properly is usually well controlled thereby allowing for an improved quality of life.
– Nasal polyps
Nasal polyps are soft, painless, noncancerous growths on the lining of your nasal passages or sinuses. They result from chronic inflammation and are associated with asthma, recurring infection, allergies, drug sensitivity or certain immune disorders. Small nasal polyps may not cause symptoms but larger growths or groups of nasal polyps can block your nasal passages or lead to breathing problems, a lost sense of smell and frequent infections. Nasal polyps can affect anyone, but they’re more common in adults. Medications can often shrink or eliminate nasal polyps, but surgery is sometimes needed to remove them. Even after successful treatment, nasal polyps often return therefore it is necessary to have close follow-up with an Allergist to monitor your condition.
– Aspirin Exacerbated Respiratory Disease (AERD): aspirin desensitization
AERD describes patients with asthma and chronic rhinosinusitis (CRS) with nasal polyposis, who experience acute upper and lower respiratory tract symptoms following the ingestion of aspirin or other NSAIDs. AERD affects 5-20% of all patients with asthma. Reactions to NSAIDs typically begin 30 minutes to three hours after ingestion and present as a sudden worsening of asthma and nasal congestion. Aspirin desensitization followed by daily aspirin therapy may be beneficial in carefully selected patients with AERD and one of the following disorders:
- Nasal polyposis that is worsening or recurring despite intranasal glucocorticoids and other appropriate therapies.
- Inflammatory conditions requiring daily NSAID therapy that cannot be treated with selective COX-2 inhibitors.
- Atherosclerotic heart/vascular disease requiring the antiplatelet effects of aspirin.
- Recurrent headaches or other conditions requiring intermittent use of NSAIDs.
Aspirin desensitization is performed in the office with close observation. Following desensitization, patients must ingest aspirin or an NSAID daily to maintain the desensitized state. The choice and dose of aspirin or NSAID for ongoing therapy depends on the indication for desensitization. As long as the desensitized state is maintained, the patients can tolerate different COX-1-inhibiting NSAIDs interchangeably.
Chronic Urticaria (hives) and Angioedema (swelling)
– Chronic Spontaneous Urticaria (CSU)
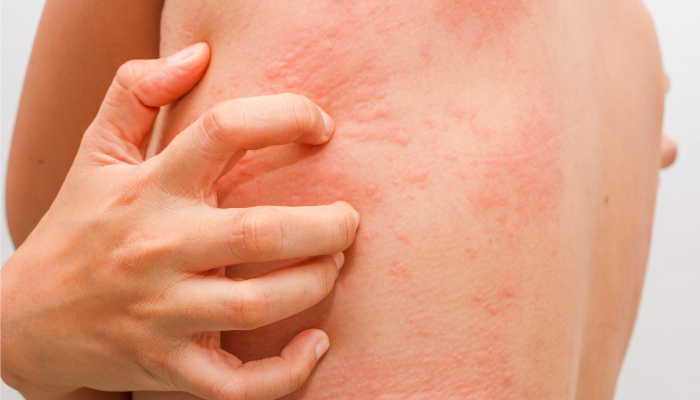 CSU is the medical term for chronic hives that have no known cause. It can look and feel different for everyone, but all cases of CSU result in itchy hives that last for six weeks or longer. This can result in raised red bumps that may grow, spread, change, disappear and reappear on the skin. Unlike other types of hives, there is no known cause of CSU. This makes it harder to diagnose and treat than other conditions, and it may take some time before you are diagnosed. If you think you might have CSU, speak with an allergist, who is trained to identify and diagnose the cause of hives.
CSU is the medical term for chronic hives that have no known cause. It can look and feel different for everyone, but all cases of CSU result in itchy hives that last for six weeks or longer. This can result in raised red bumps that may grow, spread, change, disappear and reappear on the skin. Unlike other types of hives, there is no known cause of CSU. This makes it harder to diagnose and treat than other conditions, and it may take some time before you are diagnosed. If you think you might have CSU, speak with an allergist, who is trained to identify and diagnose the cause of hives.
CSU is not caused by allergies or an infection, and it is usually not life threatening. It also is not contagious and it is not caused by a reaction to the sun, stress, hormones, foods or other medical conditions. While some people may identify things that make their CSU seemingly worse, what distinguishes CSU from other forms of hives is that there is no known cause.
People who have chronic hives often think the hives are caused by something they’ve done or interacted with. Many people will go through an “elimination diet,” meaning they take foods out of their diet and slowly add them back to see if they have a reaction. They may also try to change products like soaps and detergents. For people with CSU, these things won’t make their hives go away.
– Idiopathic Angioedema
History of intermittent swelling episodes with an unknown trigger could be a sign that you are suffering from chronic idiopathic angioedema (CIA). CIA may be associated with hives but does not have to be. Common triggers include heat, cold, and viral infections. CIA is more common in females with an average age of onset between 30-50 years. Plasma and tissue factors, such as bradykinin, have been associated with angioedema.
– Hereditary Angioedema (HAE)
Hereditary Angioedema (HAE) is a very rare and potentially life-threatening genetic condition that occurs in about 1 in 10,000 to 1 in 50,000 people. HAE symptoms include edema (swelling) in various parts of the body, including: hands, feet, face and airway (throat). Patients often suffer excruciating abdominal pain, nausea, and vomiting caused by swelling in the intestinal wall. Swelling of the airway or throat is particularly dangerous, because it can cause death by choking. It is common for HAE patients to remain undiagnosed for many years. HAE symptoms are not the same for every person, even within the same family. Therefore, patients must partner with an HAE treating specialist, like those at Bernstein Allergy Group, to create an individualized treatment plan that leads to a healthy life.
– Acquired Angioedema
Eczema
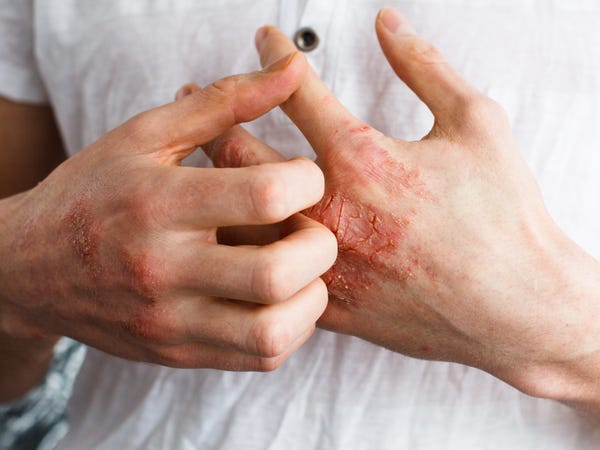 Eczema is the name for a group of conditions that cause the skin to become itchy, inflamed, or have a rash-like appearance. There are several types of eczema including atopic dermatitis, contact dermatitis, dyshidrotic eczema, nummular eczema, seborrheic dermatitis, and stasis dermatitis. Eczema is very common. In fact, over 31 million Americans have some form of eczema. Eczema can begin during childhood, adolescence, or adulthood and it can range from mild to severe. While the exact cause of eczema is unknown, researchers do know that people who develop eczema do so because of a combination of genes and environmental triggers. When an irritant or an allergen from outside or inside the body “switches on” the immune system, it produces inflammation. It is this inflammation that causes the symptoms common to most types of eczema. Eczema is usually itchy. For many people, the itch can range from mild to moderate. But in some cases, it can become much worse and you might develop extremely inflamed skin. Sometimes the itch gets so bad that people scratch it until it bleeds, which can make your eczema worse. This is called the “itch-scratch cycle.” There is no cure for eczema but there are treatments. Depending on age and eczema severity, these treatments include over-the-counter (OTC) remedies, prescription topical medications, phototherapy, immunosuppressants and biologic drugs. Many people with eczema also find success with specific natural and alternative treatments. The National Eczema Association is a great resource for more detailed information about eczema.
Eczema is the name for a group of conditions that cause the skin to become itchy, inflamed, or have a rash-like appearance. There are several types of eczema including atopic dermatitis, contact dermatitis, dyshidrotic eczema, nummular eczema, seborrheic dermatitis, and stasis dermatitis. Eczema is very common. In fact, over 31 million Americans have some form of eczema. Eczema can begin during childhood, adolescence, or adulthood and it can range from mild to severe. While the exact cause of eczema is unknown, researchers do know that people who develop eczema do so because of a combination of genes and environmental triggers. When an irritant or an allergen from outside or inside the body “switches on” the immune system, it produces inflammation. It is this inflammation that causes the symptoms common to most types of eczema. Eczema is usually itchy. For many people, the itch can range from mild to moderate. But in some cases, it can become much worse and you might develop extremely inflamed skin. Sometimes the itch gets so bad that people scratch it until it bleeds, which can make your eczema worse. This is called the “itch-scratch cycle.” There is no cure for eczema but there are treatments. Depending on age and eczema severity, these treatments include over-the-counter (OTC) remedies, prescription topical medications, phototherapy, immunosuppressants and biologic drugs. Many people with eczema also find success with specific natural and alternative treatments. The National Eczema Association is a great resource for more detailed information about eczema.
Rare Diseases
– Mastocytosis, Idiopathic Mast Cell Activation Syndrome (MCAS)
– Seminal Plasma Hypersensitivity
 Allergic reactions to human seminal plasma (HSP) or male semen may present with either localized-vaginal reactions, systemic-allergic reactions (including anaphylaxis), or both. While HSP allergy is rare, it may be underreported because of the socially-sensitive nature of the problem or misdiagnosed as vulvovaginitis. This disorder occurs exclusively in women, most typically between the ages of 20 and 30 years of age. Signs and symptoms begin shortly after ejaculation, typically during or immediately following the completion of intercourse.
Allergic reactions to human seminal plasma (HSP) or male semen may present with either localized-vaginal reactions, systemic-allergic reactions (including anaphylaxis), or both. While HSP allergy is rare, it may be underreported because of the socially-sensitive nature of the problem or misdiagnosed as vulvovaginitis. This disorder occurs exclusively in women, most typically between the ages of 20 and 30 years of age. Signs and symptoms begin shortly after ejaculation, typically during or immediately following the completion of intercourse.
If you believe you are suffering from allergic reactions to seminal plasma, then the physicians at the Bernstein Allergy Group might have an alternative approach that could work for you. After a thorough clinical history and investigation into other possible causes including latex allergy, the diagnosis of HSP sensitivity will be made using skin prick tests to whole seminal plasma or allergen-containing fractions of HSP in our office. While most symptoms can be prevented by the use of condoms, for women who find condom use unacceptable or wish to conceive naturally, we suggest HSP desensitization using either intra-vaginal or subcutaneous protocols.
– Progesterone Hypersensitivity
– Chronic Vulvovaginal Candida Hypersensitivity
– Dysautonomia
– Multiple Chemical Sensitivity (MCS)
Eosinophilic Disorders
 – Eosinophilic Gastrointestinal Disorders:
– Eosinophilic Gastrointestinal Disorders:
- Eosinophilic Colitis
- Eosinophilic Esophagitis
- Eosinophilic Gastritis
- Eosinophilic Gastroenteritis
– Eosinophilic Granulomatosis with Polyangiitis, aka Churg-Strauss Syndrome
– Eosinophilic Pneumonia
– Hypereosinophilic Syndrome
Immune Deficiency Disorders
 – Primary Immunodeficiency Disorders
– Primary Immunodeficiency Disorders
- Common Variable Immune Deficiency (CVID)
- Selective IgA deficiency
- Chronic granulomatous disease
- Complement deficiencies
– Secondary Immunodeficiency Disorders
 Hereditary Angioedema
Hereditary Angioedema
Hereditary Angioedema (HAE) is a disease characterized by recurrent episodes (also called attacks) of severe swelling of the skin and mucous membranes. This is a very rare and potentially life-threatening genetic condition that occurs in about 1 in 10,000 to 1 in 50,000 people. HAE symptoms include edema (swelling) in various parts of the body, including: hands, feet, face and airway (throat). Patients often suffer excruciating abdominal pain, nausea, and vomiting caused by swelling in the intestinal wall. The age at which attacks begin varies, but most people have their first one in childhood or adolescence. The frequency of attacks usually increases after puberty. Attacks most often affect 3 parts of the body and include the skin, gastrointestinal tract, and upper airway. Attacks may involve one area of the body at a time, or they may involve a combination of areas. They always go away on their own but last from 2 to 4 days. While people with HAE have reported various triggers of attacks, emotional stress, physical stress, and dental procedures are the most commonly reported triggers. HAE symptoms are not the same for every person, even within the same family. Therefore, patients must partner with an HAE treating specialist like those at the Bernstein Allergy Group to create an individualized treatment plan that leads to a healthy life.
